(A Modern Biological Adjunct in Orthopaedic Practice)
Fracture healing is one of the most remarkable regenerative processes in the human body. In most cases, bone repairs itself effectively with appropriate stabilization. However, delayed union and non-union remain significant challenges, particularly in elderly patients and those with osteoporosis. As orthopaedic practice increasingly integrates biological modulation alongside mechanical fixation, teriparatide has emerged as a promising therapeutic option.
This blog explores the science, evidence, and practical relevance of teriparatide in fracture healing.
Understanding Fracture Healing
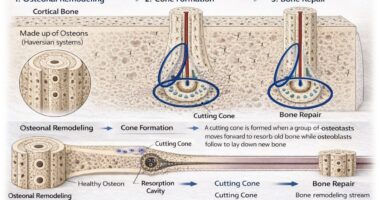
Bone healing occurs in three overlapping phases:
- Inflammatory Phase – Hematoma formation and cellular recruitment.
- Reparative Phase – Soft callus formation followed by mineralized hard callus.
- Remodelling Phase – Conversion of woven bone to mature lamellar bone.
Successful healing depends on two key pillars:
- Mechanical stability
- Biological environment
When bone quality is poor—as in osteoporosis—or when biological activity is compromised, healing may be delayed.
What is Teriparatide?
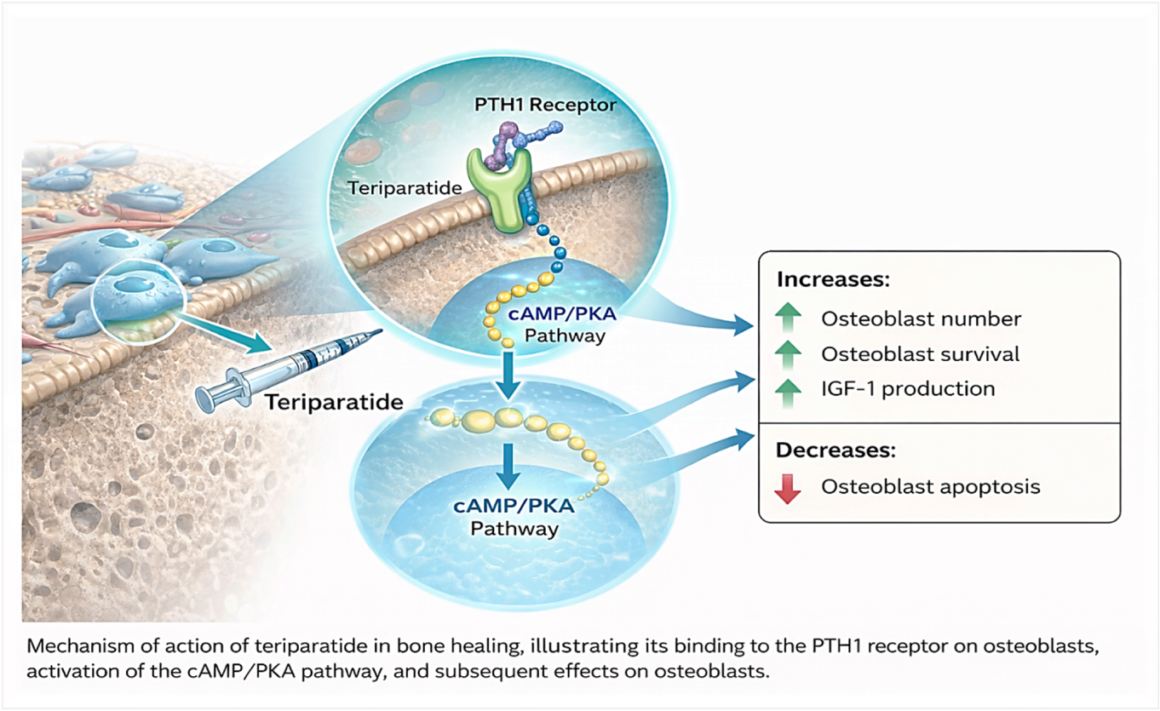
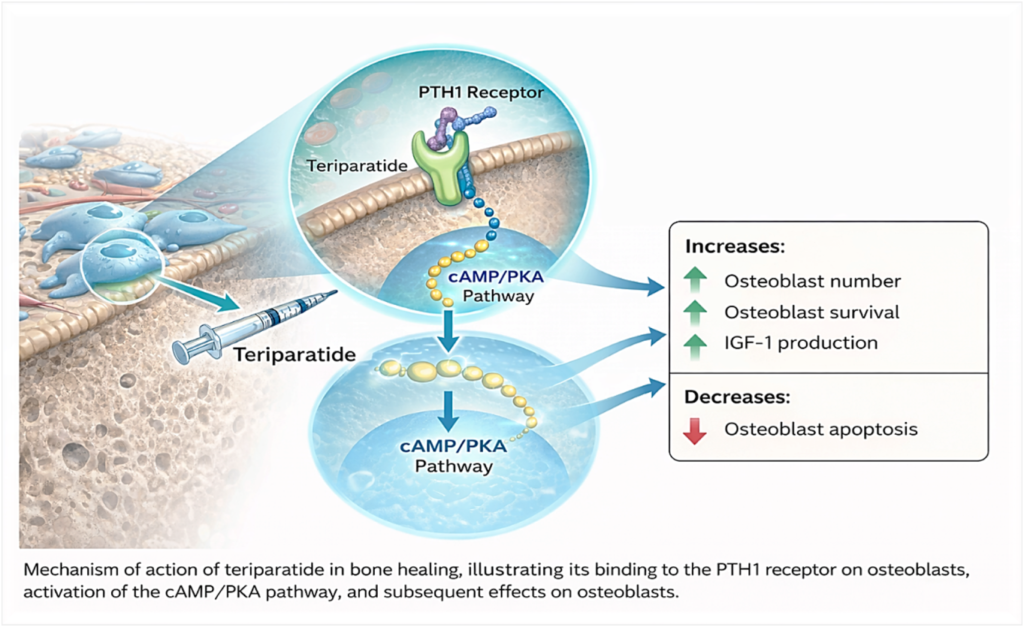
Teriparatide is a recombinant form of parathyroid hormone (PTH 1–34) and is widely used in the treatment of severe osteoporosis. Unlike antiresorptive drugs (such as bisphosphonates), which slow bone breakdown, teriparatide works as an anabolic agent—it stimulates new bone formation.
When administered intermittently (20 µg daily subcutaneous injection), teriparatide:
- Enhances osteoblast activity
- Promotes callus formation
- Improves bone mineralization
- Increases mechanical strength of healing bone
- Stimulates angiogenesis
These properties make it biologically attractive for fracture repair.
Evidence Supporting Its Role
- Osteoporotic Fragility Fractures
Clinical studies suggest that teriparatide may:
- Accelerate radiological union
- Improve pain and functional outcomes
- Enhance callus formation
Particularly encouraging results have been reported in distal radius, vertebral, and pelvic insufficiency fractures.
2. Delayed Union and Non-union
Several case series and observational studies have demonstrated union within 3–6 months in patients treated with teriparatide for delayed healing. In selected cases, it has helped avoid revision surgery.
Although evidence is promising, large-scale randomized controlled trials remain limited.
3. Atypical Femoral Fractures
In patients with suppressed bone turnover (e.g., long-term bisphosphonate therapy), teriparatide may help restore bone remodelling dynamics and enhance healing.
When Should It Be Considered?
Teriparatide is not indicated for routine use in every fracture. It may be considered in:
- Elderly osteoporotic patients
- Delayed union (no progression after 3 months)
- Established non-union with compromised biology
- Patients undergoing fixation with poor bone quality
Treatment duration typically ranges from 3 to 6 months.
Advantages
- Non-invasive adjunct therapy
- Enhances biological healing potential
- May reduce need for revision surgery
- Particularly useful in osteoporotic bone
Limitations
- Off-label use in fracture healing
- Cost considerations
- Limited high-quality randomized trials
- No standardized treatment protocol
Therefore, careful patient selection remains crucial.
The Evolving Paradigm in Fracture Care
Modern fracture management is moving beyond purely mechanical stabilization toward a combined mechanical + biological approach. Teriparatide represents an important step in this direction.
While not a universal solution, it offers a valuable adjunct in biologically compromised fractures. As further high-quality studies emerge, its role may become more clearly defined.
Final Thoughts
Teriparatide has opened new possibilities in fracture healing, particularly in osteoporotic and delayed union cases. With judicious use and proper patient selection, it can serve as a powerful biological enhancer in orthopaedic practice.
As fracture management continues to evolve, integrating anabolic therapy with sound surgical principles may represent the future of optimized bone healing.